

Following a request for some information on ‘Necrotising Soft Tissue Infections’ (NSTI’s), or more commonly referred to as flesh eating bacterial infection, we scoured our own articles first, which highlighted that we don’t have a specific dedicated article to this subject.
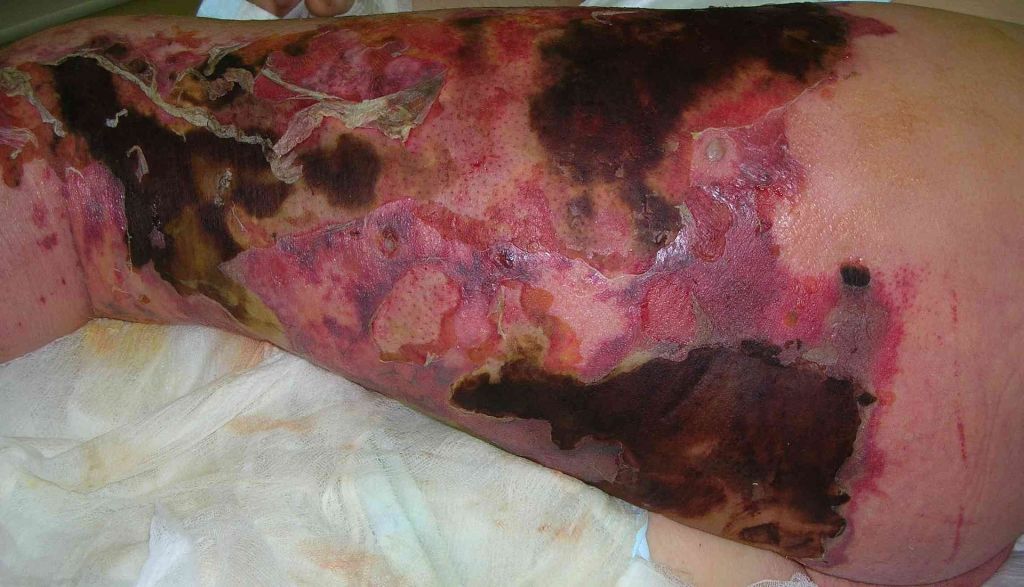
We also chose the lead image as a rather benign image of Staphylococcus Aureus, one of a few bacteria responsible for this condition. Ordinarily we shy away from sharing graphic images but felt on this occasion it was warranted to include a more graphic representation of what this condition looks like. We did however decide to bury them in the text to try and avoid them being the lead social media thumbnail. Any Google search will find no shortage of similar and much more graphic images, but it is important to show just how serious this condition is.
We will add our own article in due course though. We do however cover similar types of conditions in a few other articles including the articles on hypoxia, wound healing, and gas gangrene because of shared pathologies and similarities, specifically the gas gangrene article.
Instead today we share the indication article directly from the Undersea & Hyperbaric Medicine Society (UHMS) who advise health authorities around the world. Remembering of course that a medical “indication” is the term used when a specific treatment is appropriate and justified for a specific condition.
The UHMS state:
“Hyperbaric oxygen therapy is a recognized accepted adjunct to surgical debridements, antibiotic therapy and maximal goal-directed critical care therapy for infections of soft tissues resulting in necrosis.”
Undersea and Hyperbaric Medicine Society. (HYPERBARIC OXYGEN THERAPY INDICATIONS: 13th EDITION – 2014)
Rather than reinventing the wheel at this time, their article makes for good reading regarding the rationale behind commissioning HBOT as an adjunct therapy in what can amount to an emergency condition. Oxygen is a powerful anti bacterial as we discuss in many of our own articles and the use of HBOT comes highly recommended, especially in cases where aggressive antibiotic therapy returns poor results and tissue necrosis is progressive.
Currently however, the NHS Commissioning Board in the UK seem to disagree with the experts on this one as is evident in their commissioning document for HBOT and necrotising soft tissue infections. And please note that the board are regarded separately from the hard working frontline staff of the NHS itself whom we love to the ends of the earth.
The board conclude:
“NHS England has carefully reviewed the evidence to treat necrotising soft tissue infection with hyperbaric oxygen therapy. We have concluded that there is not enough evidence to make the treatment available at this time. “
Notwithstanding that, herewith a reliable standardized trial entitled:
Hyperbaric oxygen therapy for necrotizing fasciitis reduces mortality and the need for debridements.
Published almost 30 years ago, it is surprising how behind the curve the decision makers up the ladder still are. It, and the authors are not alone in their conclusions, conclude the exact opposite as quoted:
“The addition of HBO therapy to the surgical and antimicrobial treatment of necrotizing fasciitis significantly reduced mortality and wound morbidity (number of debridements) in this study, especially among non clostridial infections. We conclude that HBO should be used routinely in the treatment of necrotizing fasciitis.”
Another study of interest involving an impressive 1583 patients with NSTI’s published in 2014 by Joshua J Shaw et al, entitled:
Concludes:
“At HBOT-capable centers, receiving HBOT was associated with a significant survival benefit. Use of HBOT in conjunction with current practices for the treatment of NSTI can be both a cost-effective and life-saving therapy, in particular for the sickest patients.”
We will circle back to this subject in due course for a more thorough lay discussion since it one of those that the NHS Commissioning Board simply ignore the evidence on and it makes for a good policy and political bunfight as well. In the meantime the UHMS article explains the physiology and benefits that can be derived from HBOT.
Of course we can do our best to answer questions and direct readers to further online resources.
©Hayden Dunstan





1 thought on “Necrotising Soft Tissue Infection – NSTI”