
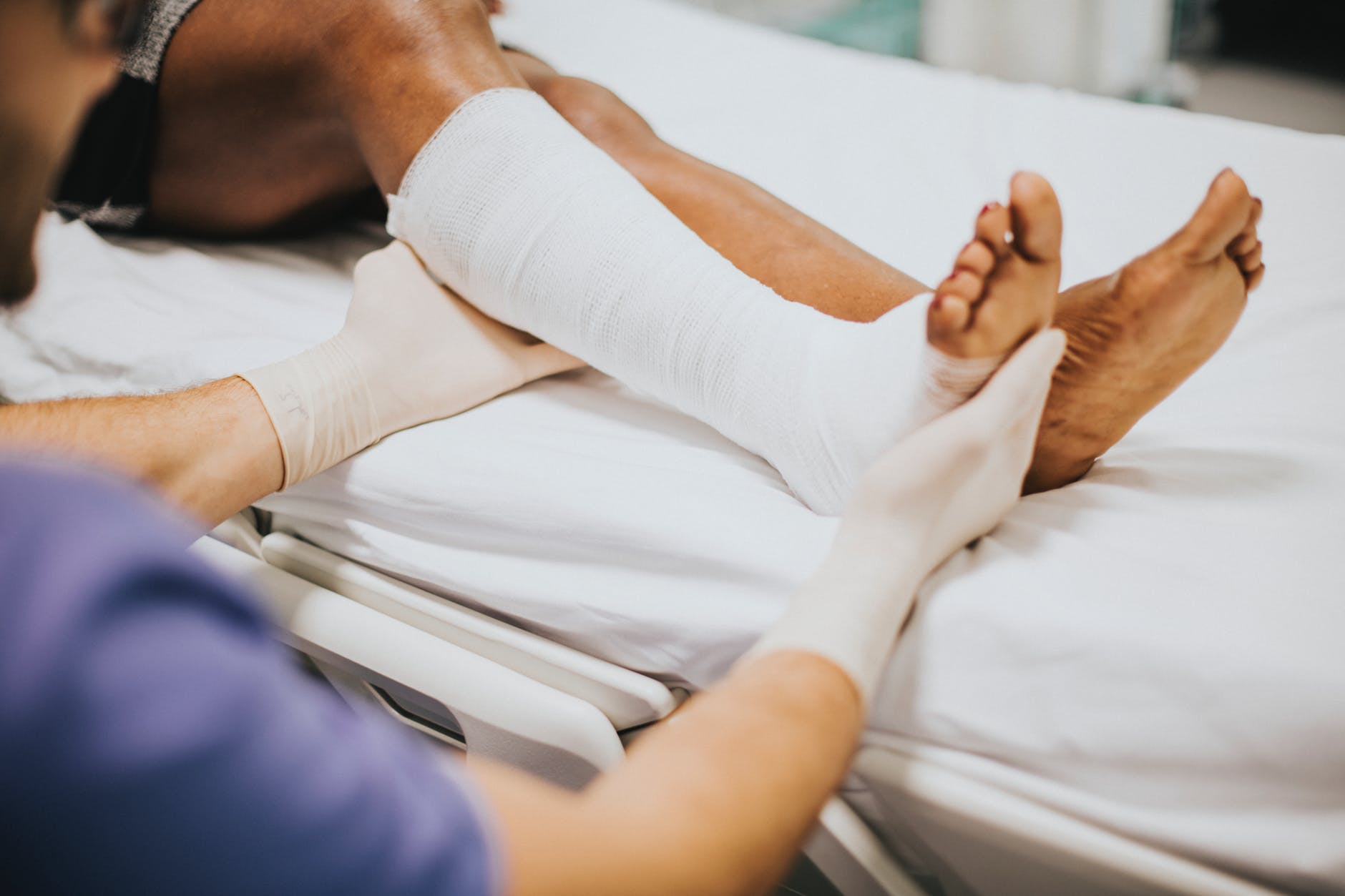
Presenting a slightly shorter read today we address wound healing, especially problematic wound healing. We have refrained from posting graphic images of before and after wound scenarios, but these are available. In many books and papers there are comparative images taken before and after HBOT directly illustrating the improvement. Empirical evidence so to speak. We can certainly direct you to these resources if required. Personal experience also indicates that this modality works well for necrotising wounds caused by disease, accident, bites, bacteria and so on.
Oxygenation is fundamental for tissue repair and rebuilding following illness or injury. It’s what facilitates tissue granulation, collagen release and ultimately tissue re-growth. Under hyperbaric conditions this is stimulated to far higher levels. Along with a demonstrated increase in stem cell release (Thom Et al 2006 https://www.ncbi.nlm.nih.gov/pubmed/16299259 ). Wound healing is drastically accelerated when hyperbaric oxygen therapy is employed.
In cases of injury the benefits are obvious. An accelerated return to normal activity and significantly shorter periods of convalescence.
For patients who suffer from poor circulation and the subsequent poor oxygenation of tissues, this can mean the normal, or closer to normal, healing of wounds that would otherwise not heal and potentially lead to amputation.
It is well established that hyper-oxygenation increases collagen release into areas of damaged tissue. It is also established that hyper-oxygenation increases tissue granulation. (Tibbles Et al 1996; Van Neck Et al 2017 – Hyperbaric Oxygen Therapy Mediates Increased Nitric Oxide Production Associated with Wound Healing: A Preliminary Study -Boykin Et al 2007) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5467109/
We’ve mentioned horses previously. Hyperbaric oxygenation is widespread in the equine field with hyperbaric oxygen therapy given to increasing numbers of horses, to accelerate their healing after sustaining injuries. The reason horse owners invest the money they do in hyperbaric chambers is clear. It works. It’s as simple as that. The point being made is that in a situation where accelerated healing is needed it is achieved using hyperbaric oxygenation. Visit the link for the Equine Hyperbaric Center for more info. https://equinehyperbariccenter.com/. They have case studies published involving injury and wound healing which involve a lot more than racing. Animal welfare certainly takes the foreground.

The mechanism of HBOT which accelerates and assists healing of non-healing wounds is described as follows:
With increased cell metabolism and greater uptake of ATP (adenosine triphosphate, the energy molecule in cells), cell mitosis and division are accelerated. Type 3 Collagen is also released in greater quantities allowing the formation of the extra cellular matrix developed by fibroblasts. This results in quicker and better granulation in the wound bed, and along the wound margin, and quickens the development of natural scaffolds on which yet more tissue can grow with improved cell division and growth. Eventually, long stranded, stronger type 1 collagen forms on the natural matrix scaffold leaving a scar. I.e. the wound heals as it would have done in normal circumstances, but would fail to do, if vascularisation was compromised and hyper-oxygenation wasn’t applied.

HBOT also triggers new vascularisation (neovascularisation), angiogenesis and vascular growth. (Hyperbaric Oxygen Therapy (Review) Tibbles Et al 1996)
Mention was made in the article ALTITUDE, THE HYPEROXIC HYPOXIA PARADOX, AND THE COMMON SENSE PARADOX of the Hypoxia Inducible Factor Gene Alpha 1. HIF1A as the master regulator gene responsible for the up-regulation of around 60 other hypoxia triggered genes. One of those factors is the Vascular Endothelial Growth Factor or the VEGF. This is a signal protein responsible for triggering new vascular growth and angiogenesis following the presence of poor tissue oxygenation caused by injury, or illnesses such as diabetes for example. New capillary growth is triggered to facilitate improved oxygen delivery to healing tissue without which granulation and cell growth would remain compromised. It is well established that HBOT up regulates the VEGF allowing accelerated healing.
What’s more, in areas of severely compromised vascularisation, oxygen just cannot make it to the wound. Severe diabetic ulcers, crush injuries, burns and so on simply don’t allow for the normal passage of red blood cells. This is where oxygenation can be achieved by better saturating the plasma which can pass through far smaller structures and even increase oxygenation in other bodily fluids that can reach the site. Again, as a bridging therapy for injury, this allows tissue to survive long enough for new capillaries to grow, without which, injuries such as crush injuries and sever diabetic ulceration almost always lead to amputation.
Neovascularisation isn’t ordinarily a particularly rapid process but can be accelerated by administering HBOT which also triggers the hypoxia inducible factors as discussed yesterday in the above article. HBOT allows the body time to grow new vascular structures and blood vessels, and accelerates the growing of these vessels, while salvaging as much tissue as possible. Especially important when oxygen sensitive tissue is concerned such as the brain. In fact, it is widely accepted by researchers that microscopic issues in the brain are really just microscopic wounds and are treated the same way. We don’t treat the symptom we treat the wound at it root.

HBOT also causes a massive increase in stem cell release facilitating healing on many fronts explained further in the article STEM CELL MOBILISATION AND HBOT: CASE STUDY the above reference Thom et al refers. As we know from previous articles and references, stem cells go on to develop into new cells in areas of disease and injury as part of the natural healing process. HBOT extends the recovery envelope and stimulates exponential release of stem cells providing the tools and materials to repair and rebuild following injury, disease and wounding.
It is worth noting that In type 2 diabetics, life span following a first amputation is reported to be as little as 5 years in some cases. Avoiding amputation can extend life span for diabetic with chronic and problematic wounds.
© Hayden Dunstan


4 thoughts on “Wound Healing”