Building on previous articles about emergency medicine, severe blood loss, and even the article telling of experiments done in the 1950’s by It Borema et al, in which they removed the haemoglobin from piglets, only to have them survive in a hyperbaric environment (covered in the article LIFE WITHOUT BLOOD), today’s science bit deals with severe anaemia.
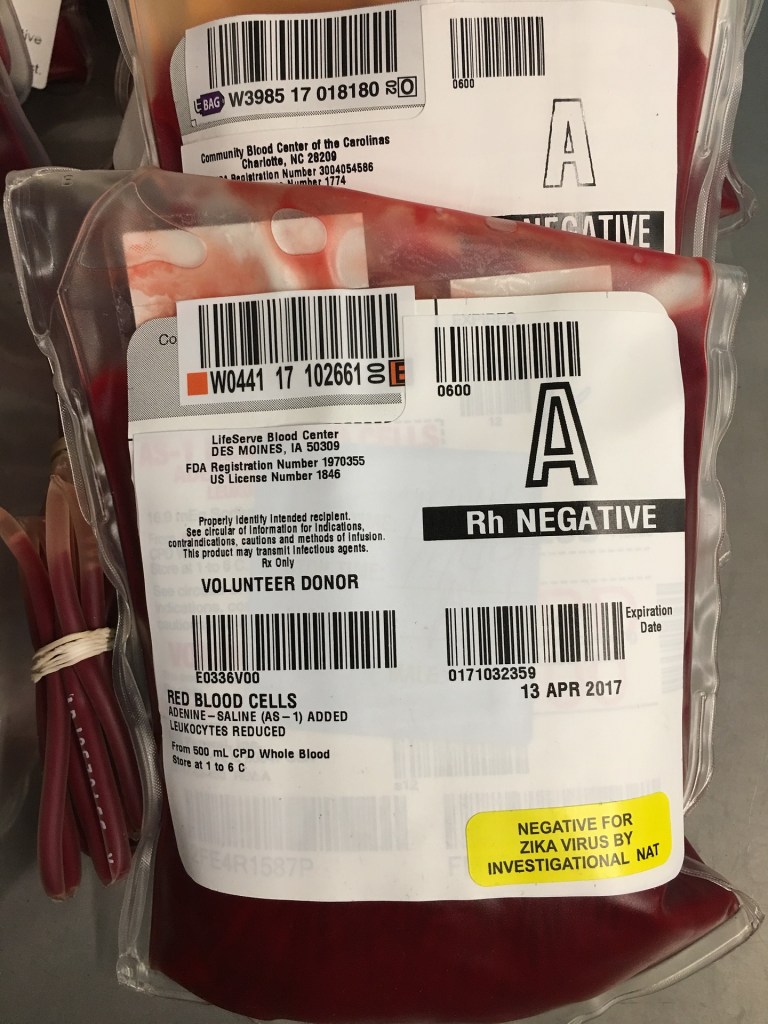
In many cases individuals may not be able to accept a transfusion in the case of massive blood loss or disease. This may be due to a number of reasons among which are medical reasons, including immunological concerns and allergies, availability, personal choice and unwillingness including religious reasons.
Whatever the reason, some patients in emergent conditions are unable to receive blood, or even plasma as it is a blood product. Today’s brief discussion explains how HBOT can contribute to better patient management in these cases. It also follows that anemia caused by other conditions may also be relieved in the same way.
Haemoglobin in the blood (protein in red blood cells), is the oxygen carrying component in the blood under normal conditions. Discussed in more detail in the article HBOT FOR CARBON MONOXIDE POISONING . A low haemoglobin count can indicate that an individual may suffer from anemia.
Symptoms common to many types of anemia include the following:
- Easy fatigue and loss of energy
- Unusually rapid heart beat, particularly with exercise
- Shortness of breath and headache, particularly with exercise
- Difficulty concentrating
- Dizziness
- Pale skin
- Leg cramps
- Insomnia
Blood loss and exsanguination share similarities with other causes of anemia, in that the blood supply no longer carries sufficient oxygen for optimal biological function.
In cases where supplemental normobaric oxygen is not enough, HBOT can provide a good bridging therapy and maintain oxygen levels during a time when blood supply is limited owing to blood loss or disease.
When blood is lost, haemoglobin is lost. Equally, if haemoglobin is lost through disease, oxygen transport is compromised. The increased oxygen debt in the body, in serious cases, can lead to permanent dysfunction of, and damage to tissues and systems. The only solution to this is to provide a pathway for more oxygen to reach tissues and cells. Ordinarily this is achieved by replacing the blood (including haemoglobin), by means of transfusion. This takes time however and sometimes needs to be an ongoing therapy for those suffering from diseases which cause anemia. It is also not always possible.
We know that blood consists mainly of plasma (water), and we know that oxygen is not particularly soluble in water under normal pressure. Plasma makes up about 55% of total blood volume. Losing half of blood volume for example, means losing half of haemoglobin volume. Resulting in critically lowered ability to transport oxygen. The remaining total volume, (plasma and haemoglobin), if it was all able to carry oxygen, would be sufficient to deliver an equivalent or higher amount of oxygen than the remaining haemoglobin alone. In the case of 50% blood loss, haemoglobin would be reduced to just 27,5% of normal blood volume. This would result in impaired oxygen transport.
As we know, HBOT exponentially increases the oxygen carrying capability of plasma. As shown in experiments, Ite Borema successfully removed the haemoglobin from piglets which then survived until being re-transfused with their own blood. Essentially, he proved that life is possible without haemoglobin at all, and survival is possible with plasma alone. Remembering that anemia is caused by a low haemoglobin count. We can indeed treat low haemoglobin count (anemia), with hyperbaric oxygenation.
So, in the event supplemental oxygen it is not enough, and doesn’t relieve anemia or oxygen debt, or for patients who don’t wish to be persistently transfused and exposed to the associated risk, what can we do? When supplemental oxygen is simply not enough to guarantee adequate oxygenation, and injury or illness seems too far gone or beyond the reach of conventional means to be remedied, or in the case of emergency intervention following trauma, we can make use of hyperbaric oxygenation as a bridge or ongoing therapy to ensure survival long enough to provide further treatment, or reduce the need for transfusion respectively.
This statement is supported by the results published by Van Meter KW (author) entitled “The effect of hyperbaric oxygen on severe anaemia.” Quoted here below:
Quote: “As a respiratory pigment, haemoglobin allows blood to carry unnaturally high levels of nascent, molecular oxygen at one atmosphere of pressure in chemical solution to capillary beds and post-capillary venules supplying parenchymal cells of all organ systems in the body. When haemoglobin drops to critical levels to disallow proper oxygen delivery, hyperbaric oxygen therapy may be used as bridge therapy to emergently supply oxygen. Hyperbaric-administered oxygen allows oxygen to be dissolved in increased concentration in red blood cell-poor plasma or crystalloid/ colloid-diluted intravascular fluids in a volume-resuscitated patient.”
And:
“Hyperbaric oxygen can reduce oxygen debt decisively in the polar clinical extremes of exsanguination with cardiopulmonary arrest all the way to resuscitation of the severely anaemic patient who cannot be transfused with red blood cells for religious reasons, immunologic reasons, or blood availability problems. A hyperbaric oxygen treatment is equivalent in wholesale cost to a unit of packed red blood cells in the western world. By controversy, but true, hyperbaric oxygen provides a low-technology, cost-competitive means of pharmacologically reducing accumulated oxygen debt in the anaemic, injured or critically ill patient with little side effect. To address severe anaemia in trauma or illness, the future may well afford the use of hyperbaric oxygen therapy in the military far-forward, in pre-hospital EMS settings, in trauma centre emergency departments, in operative and recovery units, and in intensive care units of hospitals.”
https://www.ncbi.nlm.nih.gov/pubmed/23045922
Confirmed by Van Meter et al, in cases of low haemoglobin count, plasma can replace haemoglobin as the primary oxygen carrier under hyperbaric conditions, and in cases of low haemoglobin concentration, can carry sufficient quantities to sustain life and prevent further tissue damage in emergencies. It can also elevate oxygen tension for many hours following treatment as well, providing a realistic, practical, ongoing and non invasive therapy for anemia sufferers. HBOT remains a good bridging therapy for anemia and similar conditions involving vascular compromise and arterial insufficiency, as supported by the Undersea and Hyperbaric Medicine Society.
https://www.uhms.org/resources/hbo-indications.html
© Hayden Dunstan