
Taken from the overview, we return to complimentary therapy topics today with some words on Multiple Sclerosis (MS) and the power of oxygen as an anti-inflammatory. The premise of the words to follow is that MS is thought to be an inflammatory conditions cause by vascular compromise and localised brain tissue hypoxia. (Oxygen and the Brain – The Journey of Our Lifetime – Professor Phillip B James 2014)
Over 65 similar hyperbaric charities currently operate in the UK providing affordable, or free therapy to MS sufferers with incredible success. Evidence based results and case studies detailing remarkable success and improvement in quality of life abound.
MS National Therapy Centres, (MSNTC), is a charity which represents individual therapy centres across England, Scotland, Wales, Ireland, the Channel Islands and Gibraltar. These centres provide treatments, therapies, help and support to some 15,000 people living with Multiple Sclerosis, every week. It is our aim to join this family of centers at least as it relates to the type 3 services we plan to offer.
Inflammation:
Any discussion about HBOT and wound healing wouldn’t be complete without mention of inflammation. Uncontrolled inflammation is the bane of all recovery efforts the body makes. Yet it is a crucial mechanism in the body’s natural immune response and repair-rebuild processes. When an injury occurs, on the back of the hypoxia induced reactions within the body, inflammation occurs. As tissue and capillaries become damaged, fluid leaks out into those tissues surrounding a wound or injury site and prevents the absorption and transport of oxygen. Since oxygen is poorly dissolved in water, (leaked fluid), cells and tissues eventually die due to localised hypoxia (lack of oxygen). This is further aggravated by the body’s response to low oxygen. It is the natural immune response to assume infection is present and to dispatch neutrophils, one of the white blood cell types, along with other white blood cells types such as leukocytes and phagocytes, to an area of low oxygenation such as an injury or diseased tissue. The programmed function of these cells is to ingest and break down foreign matter and pathogens and deconstruct cells.
Following an injury, damaged and consequentially hypoxic tissue is interpreted as foreign or pathogenic material and is deconstructed. This is evidenced by observable swelling. Redness and heat are generated by increased blood flow through the core as the body attempts to restore blood supply to the area. This leads to yet more fluid leakage into the tissues creating a rather vicious circle of further injury, this time as a consequence of excessive inflammation. Inflammation being the swelling part of it owing to additional fluid being present at an injury site. When this happens, the inflammation becomes the new mechanism of injury and it becomes imperative to control it. HBOT can and does do just that.
Much of this is covered in greater medical detail in the book shown below.

Tissue that otherwise would have survived if it were adequately oxygenated, until vascularisation could be restored, is lost. HBOT facilitates a sustained elevated oxygen tension in tissues even after a patient returns to normal pressure. This gives tissue that extra helping hand to survive and in doing so also relieves inflammation by controlling the body’s inflammatory response when it goes into overdrive.
To simplify the differentiation between injured hypoxic tissue and diseased hypoxic tissue, they are much the same for the purposes of this discussion in relation to local hypoxia. Disease could even be described as microscopic cellular injury of a sort.
For example:
In diabetic patients, sustained elevated blood glucose causes damage to the internal lining of capillaries. It sticks to them and prevents the adequate transport of oxygen through the capillary wall. This leads to local hypoxia, in essence, a microscopic injury to the blood/tissue barrier. Similar can be said of micro-emboli in the brains’ vascular system making up the blood/brain barrier. Emboli cause an opening of the blood brain barrier resulting in local inflammation following the leaking of fluid into those tissues reducing oxygen saturation, triggering the hypoxia response. Unarguably far more serious than wounds on the feet, brain disease, (micro-injury), of this nature can be very serious very quickly.
Hence, the principal for accelerated injury healing is similar to the principal of accelerated diseased wound healing.
In many cases, pain caused by an injury is twofold. It stems from obvious nerve damage occurring during the traumatic insult itself, but is also perpetuated by inflammation. So, while oxygen is not a pain killer per se, It will undoubtedly reduce pain where inflammation is present. This has been observed in the re-compression of injured divers.
Multiple Sclerosis, (M.S.), can be described as a condition of the central nervous system resulting from inflammation and subsequent de-myelination, and sclerosing, of the nerves of the brain and spinal cord. When separate incidents leading to these detectable scarred or sclerosed areas are disseminated in time, the label Multiple Sclerosis is the standard diagnostic conclusion. It’s not so much a diagnosis as it is a descriptive label. The words “Multiple Sclerosis” simply means “Many Scars”. The cause is yet unknown but it is blamed on auto-immune disease in which the immune system inexplicably attacks brain tissue. The mechanical effect of this is break down in the myelin sheath surrounding nerve cells. Demyelination is the signature of MS leading to sclerosis. MS causes gradual destruction of myelin (demyelination) and transection of neuron axons in patches throughout the brain and spinal cord.
The assertion that it’s ‘inexplicable’ however is not agreed upon by all. Some disagree , citing one potential cause as being a compromise of the blood/brain barrier, which triggers the fluid/inflammation response already discussed. Immune response is involved, but not inexplicably. It comes into action when the tissues surrounding a blood/brain barrier compromise become inflamed following fluid leakage. The hypoxia induced response then kicks in as discussed under wound healing. It’s the causes of these incidents of blood/brain barrier compromise that may well at a future time offer up a better understanding of M.S. Something as seemingly benign as a remote site injury, leading to micro emboli in the circulation, could very well be involved.
One incidental effect of HBOT is that as oxygen tensions rise in the blood, less oxygen debt exists in the body. This leads to blood vessels not dilating as much as they may normally do. Being permeable by design, blood vessels become more permeable when they over dilate and the opposite of this is true as a direct result of hyper-oxygenation. The blood vessels throughout the body become less permeable, further reducing the inflammatory and hypoxia response. More on blood vessels here:
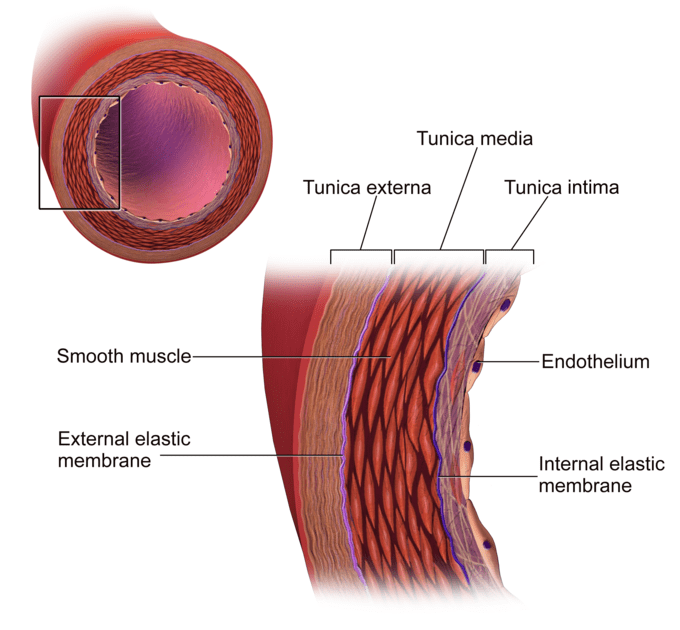
MS cannot be cured with HBOT, but it is certainly a great management tool, and indeed there are over 66 charity units operating across the UK under the auspices of The Hyperbaric Oxygen Treatment Trust, and, Multiple Sclerosis National Therapy Centres. These are charitable centres run by volunteers and have assisted in millions of safely executed treatments over recent years.
Hayden Dunstan




4 thoughts on “Oxygen as an Anti-Inflammatory and Multiple Sclerosis”