So we’ve been a little quiet lately on the writing front. This is due to an upcoming move. After 10 years in one place, it’s time for a change. Accordingly, rather than writing broken biscuits from a distracted mind, I left it out for a bit.
Today however, I found this one I had worked on before. I’ve been asked many times what the side effects of HBOT are. And what conditions might prevent a person from being deemed fit to undergo pressurisation. A contraindication is something that goes contrary to a person’s indicated suitability for somehting. It’s not a specific HBOT term, it applies to all medicine. Some people just can’t have some medicine and equally so, some people, albeit very few, just can’t have HBOT.
That said, generally speaking, and in the words or Professor Philip B James, professor of hyperbaric medicine at the Wolfson Hyperbaric Unit at the University of Dundee, if you’re fit to fly, you’re fit to recieve HBOT.

These are those things. There aren’t many to be honest. With perhaps one or two outright contraindications most are what are called “relative contraindications”, which means that with the appropriate management they are not an outright barrier to receiving treatment.
As a general rule HBOT is perhaps one of the safest therapies around. So much so type 3 HBOT was deregulated by act of parliament in 2008 with explanatory notes here
Side Effect: Temporary Myopia
Eyesite can deteriorate temporarily following multiple treatments. Any near sightedness or myopia experienced is reported to reverse spontaneously after approximately 6 weeks. Do not have your prescription adjusted if you wear glasses. This will spontaneously reverse. Notwithstanding that, retinal oxidative stress can cause problems and dosage must be considered if treating conditions of the macular and newborns. Low dose treatments (in the region of 1,5 to 1,75 ata) are recommended to avoid oxidative stress, although the body’s response to reactive oxygen species is documented and the body readily recovers from any such stress after the first treatment as discussed in the article OXIDATIVE STRESS, FREE RADICALS, RONS AND DIABETES . This rings of the toxicity fear though. In routine doses toxicity is extremely rare. Obviously always consult a doctor and make sure you are medically fit to go under pressure.

Risk: Dysbaric Injury
is always a possibility when going under increased pressure and then returning to normal pressure, with middle ear barotrauma (pressure induced injury) being the most common occurrence of this. Although not common, in fact, very rare. With changes in volume of air spaces, as described under the heading, Boyle’s Law in the downloadable overview, gas contracts and expands proportionately with the pressure applied to it. Failure to adequately equalise the ears, sinuses, lungs and other air spaces can result in injury, or barotrauma as it’s called in diving. This is easily managed by equalising air spaces and stopping the pressurisation if this proves problematic. Patients with devices containing air spaces that are not able to be equalised may be contraindicated since these devices can crush under pressure if not equalised. The same applies to any device taken into the chamber. It is advisable to leave your phone in a locker for this reason. Notwithstanding that, most pacemakers are rated to pressure of 2,5ata. Check manufacturer specs though. We aren’t pacemaker experts. A full section on this feature can be found in the British Hyperbaric Association safety documentation as well as our upcoming training and resource manual, and is well worth a read.
Poorly filled teeth can experience a form of barotrauma as well. If air can collect behind a filling then it is generally assumed that it can escape, and usually does. In worst case scenarios though, fillings can come loose with or without minor pain. On my first chamber run ever I lost all the fillings in my mouth at once. It wasn’t that bad. I did find a new dentist though. Again, a rare occurrence unless your dentist was like mine. If you’re a regular rider, let your dentist know when they’re doing fillings, they are generally only too happy to pay a little more attention to air spaces.

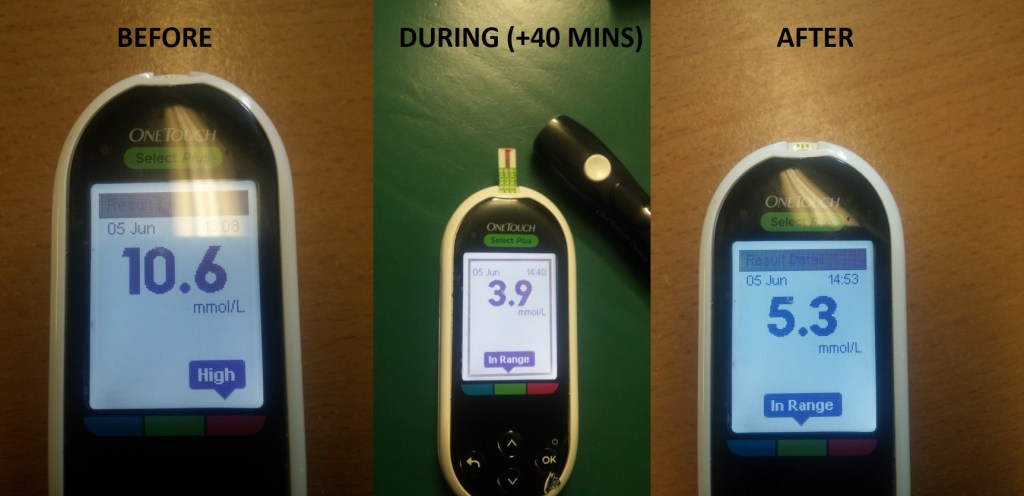
Side Effect: Lowering of Blood Glucose
Certainly, a side effect to take note of. Effectively managed by eating before a treatment to maintain a normal or even slightly elevated blood sugar level. Non-diabetics needn’t worry, the body is pretty good at balancing its own sugar. Diabetics are advised to be aware that blood sugar may drop following an increase in insulin sensitivity. This well known effect is the basis for the hypothesis in 3 parts starting with HYPERBARIC OXYGEN THERAPY DIABETES / OBESITY HYPOTHESIS – PART ONE…
Type 2 diabetic patients will often have higher than normal insulin levels. This is due to insulin resistance, and the failure of cell gateways to open in the presence of the hormone. The hormone then builds up to higher than normal levels because it’s not being used. Hyperbaric oxygen increases insulin sensitivity and gateways open suddenly allowing elevated levels of naturally produced insulin to be made available to cells and can rapidly lower blood glucose. Many diabetics will be advised to take a non-powder snack in to the chamber with them or a sweetened drink just in case. It’s that easily managed.
Side Effect: Fatigue
Following blood glucose level reduction, patients can experience fatigue, especially after repetitive treatments. Also, the increased uptake of the energy molecule ATP (adenosine triphosphate) gives the cells a bit of workout, and while not immediately noticeable like a gym workout is, owing to this not being connected to the sympathetic nervous system, fatigue is possible. Handy if you’re an insomniac suffering from sleep deprivation and the resultant anxiety associated with that. Also better discussed in the article SLEEP – THE ELIXIR OF LIFE

Side Effect: Reduced Cardiac Output
HBOT is known to cause mild vasoconstriction. It’s the basis for claims that it supports protection of the blood/tissue and blood/brain barrier. It constricts blood vessels slightly rendering them less permeable and less leaky. Unlike interventionist vasoconstriction, ie. taking a medicine to constrict vessels, vessels constrict because the circulatory system is now transporting exponential amounts of oxygen and therefore does not need to work as hard. It gets a rest so to speak. The very natural result of this is vasoconstriction much the same as happens when asleep, and the brain will likely signal the heart to beat a little slower and cardiac output will be reduced slightly. This not ordinarily a problem, however patients with an ejection fraction lower than 35 are contraindicated for treatment. This is usually from a weak heart muscle or compromised cardio system.
Risk: Pulmonary and Central Nervous System Toxicity
Explained in detail in the three part series starting with OXYGEN TOLERANCE – MYTH VS FACT – AN INTRODUCTION TO A THREE PART SERIES. This is easily managed by observing recommended exposure limits and by scheduling air breaks at regular intervals as recommended by the Repex method. Any reputable hyperbaric unit will only operate well within these limits anyway. It is not a concern for the patient to worry about.
Side effect: Slight Increase in Blood Pressure
Increased pressure acts against the blood pressure causing a small increase in values. Bear in mind that in a dry environment, redistribution of fluid in the body is not usually observed. This is uniquely experienced in a wet environment. The added pressure will however reduce edema. Unless a patient has an exceptionally high and untreated blood pressure (untreated hypertension), this does not present a problem. This would be covered in a pre-admission medical exam or inquiry in any event. In some rare cases, patients with chronic kidney disease are contraindicated because increased blood pressure can be problematic.
Side Effect: Cataracts
Unlike tumours, cataracts will grow with hyperbaric oxygenation unfortunately. There’s no two ways around it. These can however be removed surgically, and if the benefit outweighs the risk, go for it. Cataracts will not spontaneously develop however. They will only grow if you already have them.
Side Effect: Otitis media.
The inability of fluid to drain in the middle ear. Usually as a result of some kind of ear or sinus infection. This can be relieved in the chamber with a long-lasting decongestant but will drain eventually, with only a slight muffling of hearing. Since fluid is relatively incompressible and not subject to Boyle’s law, barotrauma will not occur. A good rule of thumb is if you have a severe infection of any part of the respiratory system, rather sit out that day. Air passage blockage can result in barotrauma above.

Contra Indication: Chronic Emphysema
This is a disputed one with some physicians taking the position that it’s not a contraindication because HBOT treats emphysema. Reduced lung surface area from damaged alveoli can result in it being mechanically harder to catch your breath under external pressure. This can be distressing however will cause no actual harm. Ask your doctor, or more accurately, ask the right doctor. A specialist will have knowledge of what effect HBOT may have on and individuals specific lung disease. Many claim this is an outright contraindication based on the belief that free radicals cause further lung damage. This too is disputed. See the article OXIDATIVE STRESS, FREE RADICALS, RONS AND DIABETES.

Contra Indication: Certain Chemotherapy Drugs
Some chemotherapeutic agents are reportedly contraindicated. Daunorubicin, Bleomycin and Bisulfan among them. Some will, some won’t. That said, HBOT is also used as a chemo-facilitator and improves the targeting of drugs such as SMA–pirarubicin (Moen et al. 2012 HBO and colorectal cancer). It is thought that some chemotherapy drugs can increase the risk of pulmonary toxicity. Those that present an unacceptable risk of pulmonary toxicity should be stopped for the duration of treatment and can be resumed a few days after completion. Consult with a hyperbaric doctor to make sure any chemotherapy being administered is not contraindicated. Unfortunately most doctors without a hyperbaric specialty don’t know. Specialist advice is advised. Although, there is recent research which is contrary to this as a contraindication which reports chemo-facilitation and increased chemo receptiveness is facilitated by HBOT. This demonstrates the division within the HBOT community. Clinical evidence supports HBOT as a chemo facilitator yet still some distance themselves from this and include it in contraindications.

Contra Indication: Untreated Pneumothorax
For obvious reasons an untreated collapsed or ruptured lung is contraindicated for treatment. Especially where air is present in the chest cavity. The pressure/gas relationship prevents safe treatment. It would indeed reduce the volume of air in the chest cavity in the case of a ruptured and collapsed lung, but it would also cause compressed air to expand upon releasing of pressure. Therefore, potentially adding compressed air to the chest cavity through the lung rupture is dangerous.
Releasing air from the chest cavity can more easily be achieved with a simple chest drain or tube which would, in the case of a diving injury, be inserted by a diver medical technician while under pressure mitigating the risk. In the event a diver has a collapsed lung, and a diving doctor is unavailable, a supervisor or medic would need to decide on a course of action based on whether the risk of arterial gas embolism (AGE) outweighs any risk in recompressing. The US Navy says, “When in doubt recompress”. But that’s for divers. As a general rule in diving, pulmonary barotrauma is treated the same way as decompression sickness and grouped under the term “decompression illness”. But really only because a drain is inserted in the chest during treatment to allow expanding air to escape. Non-diver patients with untreated pneumothorax are absolutely contraindicated. This is thought to be the only outright contraindication. If a pneumothorax has been treated successfully, it will likely be safe to compress a patient.

Relative Contraindication: Hernia
Hernia is also one of the disputed contraindications for use of HBOT. Abdominal Wall Hernia and Diaphragmatic Hernia are examples of hernia that may be contraindicated, especially if the are strangulated.
The thinking is that any air that may be swallowed, (and people swallow air more often than not), may expand and cause dysbaric injury in the intestines, stomach or guts as above.
The problem with this thinking is that HBOT patients seldom breathe air. They breathe oxygen and oxygen dissolves directly into abdominal wall tissue in relatively short order. At the most, 5 or 10 minutes is sufficient to dissolve a swallowed pocket of oxygen through the abdominal wall. For this reason we adopt very slow depressurization protocols to allow any swallowed oxygen to dissipate into the body. We depressurise slower than than the time required for oxygen to dissolve into tissue.
The problem comes if an individual breathes air from the chamber atmosphere, and swallows this. The inert nitrogen component in air does not dissolve into the abdominal wall like oxygen does.
Hernia is contraindicated for diving because divers for the large part breathe air or other inert gas diluent. In HBOT patients breathe oxygen for the large part and even if the patient swallows air on the last air break, any oxygen breathed following that will displace the inert gas and the oxygen will be absorbed as it does in lung absorption.
Ordinarily, a 15 minute decompression time is observed and this is ample to eliminate any gaseous oxygen that may have become trapped in a herniated bulge through the abdominal or diaphragmatic wall.
Notwithstanding all of that, almost all swallowed air doesn’t become trapped and the risk of this being an issue is so low it is considered insignificant for oxygen treatments. Most swallowed air will find it’s own way out the top… or indeed the bottom, to the dismay and embarrassment of many.
For simple dry diving, it may present a contraindication until treated and resolved with surgery. More information can be found here.
Additional Considerations:
While not strictly contraindicated most facilities do not routinely administer treatment to pregnant women.
HBO may also exacerbate a high fever to a degree. A very high fever in contraindicated.
Any history of otosclerosis surgery (the stapes operation – stapedectomy) must be considered, a tube must be placed in the ear to aid equalisation.
Treatment must be stopped in the event visual impairment occurs in patients who have had optic neuritis.
Outside of the above mentioned easily managed considerations, HBOT is benign, non-invasive and safe by comparison with other rather more radical and harmful treatments commonly preferred by patients and prescribed by doctors.
This is common because HBOT is largely an unknown factor in the public awareness as well as the standard medical curriculum. Most medical professionals don’t even know what it is. It’s easier for people to default to treatments they have heard of as well. At a time in history when memes and headlines are all it takes to convince an individual, personal research is well advised. Certainly, more public education is called for. In my experience, doctors who take the time to investigate further are generally overwhelmingly convinced following research and become avid advocates for HBOT.
Everything, bar one or two contraindications above, is manageable and deemed “relative contraindications”. Those few conditions that are outright contraindications are rare. In general, most people can undergo HBOT with no significant side effects or risk.

©Hayden Dunstan